Counterfeit drugs (fake pharmaceuticals and adulterated medicines) are a growing problem around the globe. It is estimated that counterfeit medicines:
- Kill over 1 million people a year and harm many more
- Earn criminals billions of dollars each year
Counterfeit drugs also damage consumer trust in pharmaceutical products and healthcare providers. This results in poor adherence to recommended treatments, with subsequent deterioration in health conditions.
There is a mistaken belief that counterfeit medicines are only distributed in developing countries. This belief is contradicted by the growth of counterfeit medicine products in well-developed countries, as evidenced by recent counterfeit drug discoveries in Canada, Japan, the UK, the US, and Australia.
Public Health Risks & Counterfeit Drugs
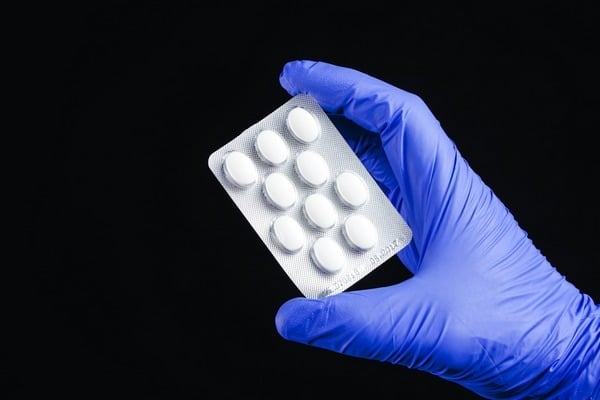
Fake medicines
Counterfeit medicines are harmful to health because they generally:
- Contain incorrect amounts of APIs (or are missing APIs)
- Contain dangerous substitutes, contaminants, and other toxic components instead of quality-controlled formulas and approved API percentages
- May lead to significant patient harm (adverse events), such as hospitalisation, disability, organ damage, or death
The World Health Organisation (WHO) estimates over 200,000 people die each year from fake malaria medicines, alone. That’s a lot of deaths linked to a single [counterfeit] product type.
Counterfeit drugs have long been a threat to patient health. Yet our populations are increasingly at risk of purchasing falsified or compromised medicines.
The issue of counterfeit medicines/falsified drugs issue is not weakening. It’s growing stronger.
With fake injectables (e.g., diabetes drugs) now circulating in medical supply chains, combined with high demand for products in short supply, we’re bound to see an increase in the number of deaths related to counterfeit medicines in the near future.
Estimates of the size of counterfeit medicine crimes (falsified medicines)
The size of any illicit market is difficult to predict with full accuracy. However, statisticians/researchers estimate the size of the counterfeit medicines problem:
- Equals from $200 billion to $430+ billion USD each year (Source: Journal of Global Health, Ofori-Parku, 2022 and World Health Organisation, et al.)
- Is increasing in size and coverage areas despite major seizures of ‘counterfeit drugs’ by Government agencies, border patrol officers, and police
- Involves counterfeit/substandard products produced and distributed by sophisticated criminal networks and unscrupulous distributors
Example: the Australian TGA recently discovered counterfeit OZEMPIC vials, an in-demand diabetes injectable used to treat obesity (i.e., semaglutide).
Why are counterfeit medicines a growing concern?
Medicine Supply Chain Issues
Some of the key factors leading to increased risks of counterfeit medicines in pharmaceutical supply chains include:
- Supply chain distribution networks: Medicine supply chains are increasingly complex
- Foreign API suppliers: Raw materials, APIs, and finished pharmaceutical products often rely on overseas suppliers, where:
- There may be inadequate compliance with GMP, GWP, and GDP
- Border-crossing distribution routes may be vulnerable to product diversions/theft or substitutions
- Medicine Shortages: World events have resulted in a variety of shortages of crucial medicines, including cardiovascular drugs, blood thinners, diabetes medicines, anti-virals, and antibiotics
Consumer Behaviours
The medicine supply chain risks listed above are further amplified by an increase in:
- The number of illicit online pharmacies
- The number of consumers shopping for discounted drug products via the internet
- Retail distributors and consumers failing to verify the authenticity/approval status of online pharmacies
- High demand for expensive drug products in short supply, including obesity treatments/injectables and anti-viral medications
Increased risks of counterfeit medicines in supply chains

It’s important for manufacturers and Regulatory Authorities to recognise that ‘counterfeit drug’ criminal organisations have become more sophisticated over recent decades.
Pharmaceutical supplies chains are at a much higher risk of:
- Product diversions/theft
- API substitutions especially in times of medicine shortages
- Infiltration by counterfeit or adulterated products
- Tampering incidents, etc.
Reducing risks and harms from falsified medicinal products
The World Health Organization, Regulatory cooperatives, and Interpol-led operations are working to disrupt criminal organisations that make or distribute counterfeit drugs. One recent police seizure of counterfeit medicinal products yielded over 300 million units of product and led to multiple arrests.
Despite major police seizures of counterfeit drugs, these medicines are a growing concern.
The problem of counterfeit medicines is worsening
Public Health Harms
Increased demand for medicines and PPE during the pandemic, along with border restrictions, led to delays in GMP compliance inspections, and difficulties with supply chain monitoring.
When it comes to counterfeit medicines, consumers and healthcare providers are often unaware of the risks of unapproved online pharmacies/other illicit distribution channels.
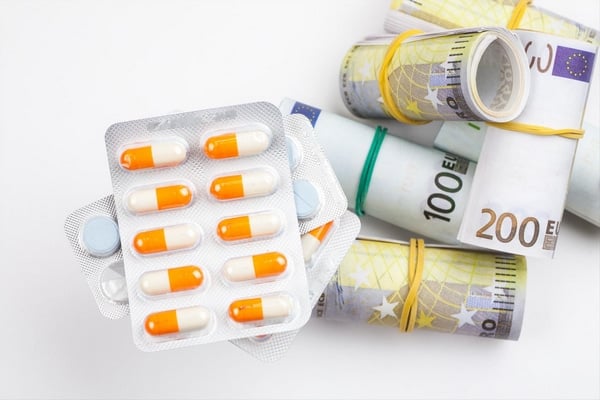
Falsified medicines (fake drugs)/counterfeits pose a major risk to patient health & safety.
In addition to reducing treatment efficacy and directly harming patients, counterfeit drug products have a detrimental impact on the industry. Counterfeit medicines, counterfeit APIs, and substandard drug products all have the capacity to detrimentally impact:
- Clinical trials and study results
- Pharmacovigilance (drug safety signal monitoring, product complaints management, SAE documentation)
- Pharmaceutical brands (reputation)
- Trust in the efficacy of a certain product type

Reducing risks and harms from falsified medicinal products
- The World Health Organization, Regulatory cooperatives, and Interpol-led operations are working to disrupt criminal organisations that make or distribute counterfeit drugs.
- Despite police seizures of millions of counterfeit medicines over recent years, the problem requires ongoing vigilance by patients, manufacturers, and regulatory auhorities.
Learn the Industry and Regulatory Authority requirements for prevention of falsified medicines/counterfeit drugs – in a GMP eLearning course on “Prevention of Falsified Medicines“.
Summary on Counterfeit Medicine Crimes
The problem of falsified medicinal products is worsening, rather than improving.
One of many contributing factors is that consumers are ordering “discount medicinal products” via unauthorised online pharmacies.
- These products are often counterfeit/falsified medicines.
- They often have inconsistent (or missing) APIs; cheaper substitute ingredients; contaminants; and other toxic components.
- Consumers and healthcare providers are often unaware of the risks of unapproved distribution channels.

Other factors leading to an increase in counterfeit drug products include complex supply chains and distribution logistics, global medicine shortages, high demand for obesity treatments, cancer drugs, and diabetes products, and ineffective pharmacovigilance systems.
For assistance with your pharmacovigilance systems, validation requirements, facility architecture/cleanroom monitoring systems, or regulatory affairs needs, contact PharmOut’s expert GMP consultants and validation engineers.
GMP Requirements & Regulations for Prevention of Falsified Medicines
If you need to learn about regulatory requirements and global prevention efforts in relation to combating counterfeit drug crimes, there’s a self-paced GMP certificate course on this topic at PharmOut’s GMP eLearning store.
The GMP eLearning course titled “Preventing Falsified Medicinal Products” will help industry and regulatory authorities prevent dangerous counterfeit medicines and other falsified drug products from entering medicinal product supply chains.
Another important GMP eLearning course is Good Distribution Practice (GDP).
These GMP certificate training courses provides learners with an overview of medicine supply chain protections, regulatory compliance requirements, and industry standards.
It is suitable for industry as well as Government agencies and:
- Includes relevant legislation and GXP requirements for preventing falsified medicinal products from entering supply chains.
- Is an ideal way to enhance your knowledge in relation to globally accepted standards such as for serialisation packaging and labelling, anti-tampering safety features, unique product identifiers (UPIs), product import requirements (medicine importation documentation requirements from non-local Regulatory Authorities), and other supply chain protection measures.
Click here to learn more about the GMP training course (a certificate course) covering the prevention of falsified medicinal products.
Need expert GMP consultancy for regulatory affairs, audit finding responses, validation activities, cleanroom monitoring, pharmacovigilance, or other regulatory compliance isssues?
Contact PharmOut’s experts for help with your pharmaceuticals, medical devices, or veterinary medicines manufacturing or importing/exporting businesses, by clicking here.
Journal Articles & Recommended Reading
Ofori-Parku SS. Fighting the global counterfeit medicines challenge: A consumer-facing communication strategy in the US is imperative. J Glob Health. (2022). Apr 23;12:03018. doi: 10.7189/jogh.12.03018. PMCID: PMC9031510.
Ofori-Parku, S.S., Park, S.E. I (Don’t) want to consume counterfeit medicines: Exploratory study on the antecedents of consumer attitudes toward counterfeit medicines. BMC Public Health 22, 1094 (2022). https://doi.org/10.1186/s12889-022-13529-7.
Aufegger, L., Yanar, C., Darzi, A. et al. The risk-value trade-off: price and brand information impact consumers’ intentions to purchase OTC drugs. J of Pharm Policy and Pract 14, 11 (2021). https://doi.org/10.1186/s40545-020-00293-
Miller, HI (M.S., M.D.) and Winegarden, W (Ph.D.), Center for Medical Economics and Innovation (ISSUE BRIEF): Fraud in Your Pill Bottle: The Unacceptable Cost of Counterfeit Medicines (2020). Published by Pacific Research Institute.
Yuen, V.W., Tang, F., Phau, I. (2018). Understanding Consumers’ High-Risk Consumption Behavior of Pharmaceuticals: An Abstract. In: Krey, N., Rossi, P. (eds) Boundary Blurred: A Seamless Customer Experience in Virtual and Real Spaces. AMSAC (2018). Developments in Marketing Science: Proceedings of the Academy of Marketing Science. Springer, Cham. https://doi.org/10.1007/978-3-319-99181-8_125
Press Release: Canadian Drug Firm Admits Selling Counterfeit and Misbranded Prescription Drugs Throughout the United States (re counterfeit cancer drugs Avastin and Altuzan) – (2018) Published by U.S. Attorney’s Office, District of Montana on 2018 April 13.
Gurney B, Amundson G, Boumediene SL.Ways to battle the $431 billion fake pharmaceutical industry. Review of Business & Finance Studies. (2017) 8:33-40.
Sato D.. Counterfeit medicines–Japan and the world. Yakugaku Zasshi. (2014).134(2):213-22. Japanese. doi: 10.1248/yakushi.13-00230-3. PMID: 24492225.
Health Canada Policy on Counterfeit Medicines: Policy on Counterfeit Health Products (POL-004). 2010.






